Hybrid natural-artificial blood vessels could also enable gene therapies and drug delivery

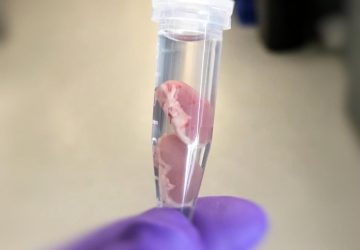
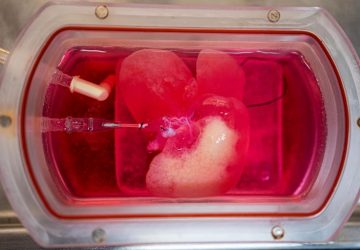
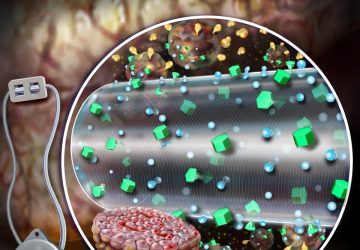
A flexible and biodegradable electronic blood vessel.
The number one cause of mortality worldwide is cardiovascular disease. Now scientists reveal electronic blood vessels might one day use electricity to stimulate healing and deliver gene therapies to help treat such maladies, a new study finds.
One-third of all U.S. deaths are linked to cardiovascular disease, according to the American Heart Association. When replacement blood vessels are needed to treat advanced cases of cardiovascular disease, doctors prefer ones taken from the patient’s own body, but sometimes the patient’s age or condition prevents such a strategy.
Artificial blood vessels that can prove helpful in cases where replacements more than 6 millimeters wide are needed are now commercially available. However, when it comes to smaller artificial blood vessels, so far none have succeeded in clinical settings. That’s because a complex interplay between such vessels and blood flow often triggers inflammatory responses, causing the walls of natural blood vessels to thicken and cut off blood flow, says Xingyu Jiang, a biomedical engineer at the Southern University of Science and Technology in Shenzhen, China. Jiang and his team report having developed a promising new artificial blood vessel that doesn’t cause inflammatory response. The scientists detailed their findings online on 1 October in the journal Matter.
To circumvent the inflammation problem, Jiang and his collaborators sought to create artificial blood vessels that combined living cells with electronics. First, they created flexible biodegradable polymer membrane sheets that encapsulated circuits made of an electrically conductive liquid metal-polymer. Next, they deposited layers of human blood vessel cells onto these sheets. They then rolled these sheets up to form multi-layered tubes whose 3-D structures resembled those of natural blood vessels.
In experiments, electrically stimulating these artificial blood vessels promoted the growth and migration of the blood vessel cells deposited in these tubes’ interior walls. Such behavior can support the formation of new blood vessels, helping wounds heal, the researchers say.
In addition, the electric fields these devices generate could make cell membranes more permeable. This in turn makes them more likely to absorb DNA for a jellyfish protein that made the cells glow green. This suggests these electronic blood vessels could support gene therapies.
In further experiments, the scientists replaced the carotid arteries of lab rabbits with the electronic blood vessels. Ultrasound imaging of the rabbits over the course of three months revealed the devices enabled sufficient blood flow the entire time, and X-ray imaging found that they appeared to function just like natural arteries, with no sign of narrowing. Afterward, when the researchers removed the implants and analyzed the rabbits’ internal organs, they found no signs that the artificial blood vessels had produced inflammatory responses.
In the future, the researchers intend to carry out longer-term animal studies. In addition, they hope to include sensors in their electronic blood vessels that can gather data on blood pressure, velocity and sugar levels. Artificial intelligence software can then analyze this data to make predictions on a patient’s health and the possible need for early interventions. “We are working on these applications at the moment,” Jiang says.
Another possible research direction is using the electronic blood vessels to deliver drugs to patients. “The drugs could be contained within the polymer part of the electronic blood vessel, or could be attached to the surface of the electronic blood vessel via some chemical modifications,” Jiang says. The devices could then electronically release these drugs once they detect problems in the bloodstream or in blood vessels. “This is an exciting area, but very costly, so we are raising funds for further work,” Jiang says.
source: www.spectrum.ieee.org