Chronic transplant rejection can be deadly, and recognising it as early as possible is key to achieving the best possible patient outcomes. Thankfully, a new test has been developed that can detect the signs of this condition in lung transplants before any outward symptoms manifest, enabling doctors to act quickly to protect their patients.
The test, which has been developed by the Laboratory of Organ Transplant Genomics in the Cardiovascular Branch of the National Heart, Lung, and Blood Institute (NHLBI), requires a simple blood sample in order to spot signs of early lung transplant rejection. Researchers believe it can potentially be expanded for use with other organs in the future.
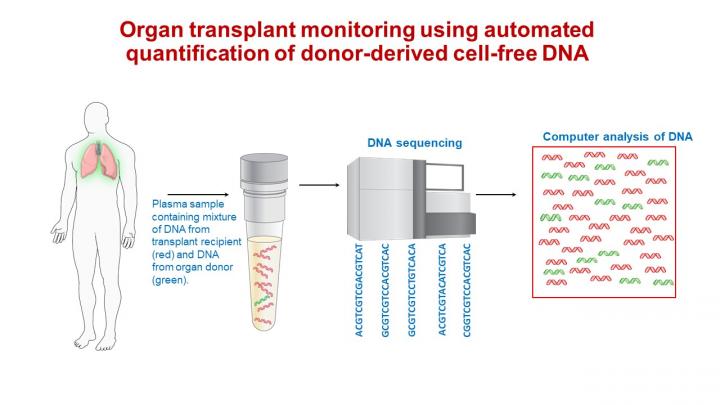
After a blood sample is taken from the arm of the affected patient, it is put into a machine that can sort the DNA fragments in the sample. Computer analysis can then be used to assess how many of these are from the patient and how many are from the donor. The more donor fragments present in the blood, the higher the risk for transplant rejection.
This was tested on 106 lung transplant patients for the first three months after they had undergone the procedure. Those with higher levels of donor DNA fragments in their blood were six times more likely to develop transplant organ failure, despite more than half of these high-risk patients showing no outward signs of rejection.
“Once rejection is detected early via this test, doctors would then have the option to increase the dosages of anti-rejection drugs, add new agents that reduce tissue inflammation, or take other measures to prevent or slow the progression,” said Dr Hannah Valentine, co-leader of the study.
This is a particularly important breakthrough because lung transplants have the lowest survival rates of all organ transplant operations. Previously, the only ways to tell if a patient was experiencing rejection before outward symptoms appeared were either invasive – like a lung biopsy – or not sensitive enough to detect the severity of what the patient was experiencing.
source: www.mediplacements.com