A study led by researchers at the University of Massachusetts Medical School has used a small interfering RNA (siRNA) to reduce preeclampsia symptoms in an animal model. This approach could provide a new way of treating preeclampsia in humans.

Hakat | Shutterstock
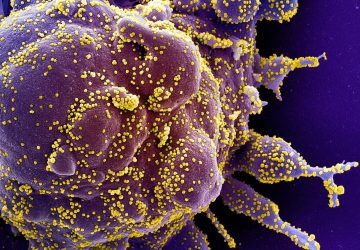
At around 20 weeks of pregnancy, women with preeclampsia develop high blood pressure and excess protein in the urine (proteinuria).
If the condition is severe, blood platelet counts fall, red blood cells break down, kidney and liver function becomes impaired and the lungs fill with fluid, causing breathing difficulties and posing a risk to both mother and baby.
The symptoms of preeclampsia are the result of a defect in the placenta that is associated with increased circulating levels of a protein called sFLT1, which serves as an on/off switch for the inhibition of new blood vessel growth.
Currently, preeclampsia cannot be cured or adequately treated and the only therapeutic option is to give birth to the baby and pass the placenta.
Professor of RNA therapeutics and study leader Anastasia Khvorova says that for women with preeclampsia, being able to carry their baby for just a few more weeks has a significant benefit in terms of health outcomes for the baby:
Thanks to rapid advances in siRNA, we’ve developed an siRNA that displays the potential to allow women with preeclampsia to extend their pregnancy from 24 or 25 weeks to as long as 30 weeks, greatly improving outcomes for the infant.”
Professor Anastasia Khvorova, Study Leader
As reported in the journal Nature Biotechnology, the researchers used the siRNA to reduce blood levels of sFLT1 in pregnant mice.
By using the compounds to target and degrade some of the messenger RNAs needed to code for the protein, the team reduced circulating levels of sFLT1 by up to 50%.
In collaboration with researchers at Sydney University Medical School, the researchers then tested the strategy in pregnant baboons, an established animal model for preeclampsia in humans. They found that just one injection of siRNA decreased circulating sFLT1 and reduced high blood pressure and proteinuria.
Khvorova says that six years ago this would not have been possible and that scientific advances enabling the chemical stabilization and production of siRNAs so that they can be delivered to tissues has led to rapid advances in these compounds: “The preeclampsia compounds we are developing are an example of what siRNA can do and how far they’ve come.”
The next step for researchers will be to secure funding for studies to further optimize the configuration of these compounds and to test their safety before approaching the U.S Food and Drug Administration for an investigational new drug application.
source: www.news-medical.net